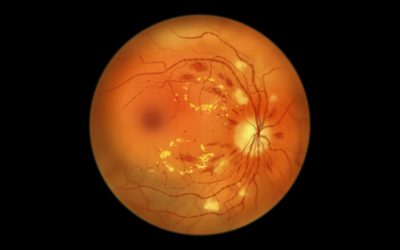
Diabetic retinopathy stands as the leading cause of new blindness cases in Americans between ages 20 and 74. This sight-threatening condition develops when consistently high blood glucose levels damage the delicate network of blood vessels nourishing your retina (the retina is the light-sensitive tissue at the back of your eye that makes vision possible).
What makes diabetic retinopathy particularly dangerous is its silent progression through four distinct stages: mild, moderate, severe, and proliferative.
What makes diabetic retinopathy particularly dangerous is its silent progression through four distinct stages: mild, moderate, severe, and proliferative. During the first two stages, you won’t notice any symptoms or changes in your vision. The condition advances quietly, causing irreversible damage before symptoms like floaters, blurred vision, or vision loss finally appear.
Recent projections reveal that vision-threatening diabetic retinopathy cases will nearly triple by 2050 as diabetes rates continue climbing worldwide. However, there is good news: Understanding how diabetic retinopathy progresses puts you in control of protecting your sight.
Early detection through regular screenings can catch this condition before permanent damage occurs. When you recognize the warning signs at each stage and understand your treatment options, you can take decisive action to preserve your vision.
Whether you’ve recently been diagnosed with diabetes or have been managing it for years, knowing how this condition advances helps you work effectively with your healthcare team to prevent vision loss.
This guide walks you through each stage of diabetic retinopathy progression, from the earliest detectable changes to advanced complications. You’ll discover the specific risks at each stage, learn when immediate intervention becomes critical, and understand the proven strategies that can halt progression and preserve your sight for years to come.
Early Signs and Non-proliferative Stages
Non-proliferative diabetic retinopathy (NPDR) represents the silent beginning of vision damage in your eyes. During this phase, your retinal blood vessels start showing the first signs of glucose-related stress. Microaneurysms, which are tiny balloon-like bulges in your blood vessel walls, begin forming as high blood sugar weakens these delicate structures over time.
Your eye doctor can spot these microaneurysms during a dilated eye exam, where they appear as small red dots scattered across your retina. These microscopic changes occur without any symptoms you can feel or see, making regular screenings your only way to catch the condition at this critical early stage.
Understanding the three stages of NPDR
NPDR progresses through three distinct phases, each creating greater risk for your vision.
Mild NPDR begins when at least one microaneurysm appears in your retina. While your vision remains unaffected at this point, you face a 5% risk of progressing to the more dangerous proliferative stage within one year.
Moderate NPDR marks a turning point in disease progression. Your retinal blood vessels begin swelling, leaking fluid, and closing off entirely in some areas. This vascular damage restricts blood flow to retinal tissue, starving these areas of essential oxygen and nutrients. The progression risk jumps dramatically: patients with moderate NPDR face a 12-27% chance of developing proliferative disease within twelve months.
Severe NPDR creates extensive blood vessel blockages throughout your retina. Your eye responds to this oxygen deprivation by preparing to grow new blood vessels, unfortunately this process leads directly to the most dangerous stage of diabetic retinopathy.
When fluid threatens your central vision
Diabetic macular edema (DME) can strike at any stage of NPDR, creating a separate threat to your sight. This condition develops when leaking blood vessels allow fluid to accumulate in your macula, which is the central area of your retina responsible for sharp, detailed vision.
DME affects approximately 1 in 15 people with diabetes. The risk varies dramatically based on your retinopathy stage: less than 6% of patients with mild NPDR develop macular edema, but this jumps to 20-63% in those with moderate to severe retinopathy.
Macular edema can be thought of as swelling that distorts the eye’s most critical vision center. Even small amounts of fluid can blur your central vision, making reading, driving, or recognizing faces increasingly difficult.
The challenge with NPDR lies in its deceptive quiet progression. Your vision may seem perfectly normal while significant damage accumulates in your retinal blood vessels.
Only regular dilated eye exams can detect these changes before they threaten your sight permanently. A comprehensive eye exam at Chang Eye Group in Pittsburgh can detect these advanced changes early and help prevent permanent vision loss.
Advanced Stages and Proliferative Disease Progression
Proliferative diabetic retinopathy (PDR) marks the point where your condition becomes critical. When blood vessels in your retina become severely damaged, your eye launches a desperate attempt at self-repair that actually makes everything worse.
Your retina, starved of oxygen due to blocked and damaged vessels, begins producing a protein called vascular endothelial growth factor (VEGF). Think of VEGF as your eye’s emergency signal, frantically calling for new blood vessels to restore circulation. Unfortunately, these new vessels grow in all the wrong places, creating a web of fragile, abnormal blood vessels that invade the space between your retina and the clear gel filling your eye.
When new blood vessels become your enemy
These newly formed vessels represent your eye’s misguided rescue attempt. Unlike healthy blood vessels, these abnormal growths have thin, weak walls that rupture easily. When they break, blood spills into the vitreous, which is the clear gel that fills the center of your eye, and causes vitreous hemorrhage.
Minor bleeding creates dark floaters that drift across your vision like small shadows. Severe hemorrhages can completely block your sight, turning your world dark without warning. Approximately 80% of patients with type 2 diabetes who experience severe vitreous hemorrhage need surgical intervention within one year.
Scar tissue that steals your sight
The abnormal blood vessels not only bleed but they also create scar tissue. As this fibrous tissue forms around the new vessels, it begins to contract like a slowly tightening rope. This contraction pulls on your retina, potentially tearing it away from the wall of your eye in what doctors call tractional retinal detachment.
Tractional retinal detachment can lead to complete blindness if not treated immediately.
Your eye can also develop neovascular glaucoma when abnormal vessels grow on your iris, blocking the normal drainage of fluid and causing dangerous pressure buildup. This complication affects approximately 3% of PDR cases. The risk of severe visual loss increases dramatically, from about 7% to over 29% in eyes with moderate to severe new blood vessel growth when vitreous hemorrhage occurs.
These complications develop rapidly and require immediate professional intervention.
Schedule a comprehensive eye exam at Chang Eye Group in Pittsburgh to detect these advanced changes before permanent vision loss occurs.
Prevention and Management Strategies
Your ability to prevent diabetic retinopathy progression lies in consistent daily habits and regular professional monitoring. Blood glucose management serves as your strongest defense against retinal damage, while early detection through screening catches problems before they steal your vision permanently.
The timing of your first eye examination depends on your diabetes type. According to the American Diabetes Association, people with type 1 diabetes should schedule their first dilated eye exam within 5 years of diagnosis, while those with type 2 diabetes need immediate screening upon diagnosis. Pregnant women with diabetes require more frequent monitoring beginning in their first trimester.
Daily habits that protect your retinal health
The National Eye Institute recommends keeping your health on TRACK:
- Take medications as prescribed
- Reach a healthy weight
- Add physical activity
- Control your ABCs (A1C, blood pressure, cholesterol), and
- Kick smoking
Strict blood glucose control makes the most significant difference in preventing retinopathy progression. Research demonstrates that a 10% decrease in HbA1c translates directly to a 39% decrease in retinopathy progression risk. Think of consistent glucose management as creating a protective environment for your retinal blood vessels.
Blood pressure control provides additional protection for your eyes. Studies reveal that managing hypertension reduces visual loss, particularly important for people with type 2 diabetes who consistently measure above 130/80 mm Hg. Your heart-healthy choices benefit your retinal health too.
Treatment options when prevention isn’t enough
Sometimes diabetic retinopathy advances despite your best preventive efforts. When this happens, proven treatments can halt progression and preserve your remaining vision. Anti-VEGF injections target the proteins that cause abnormal blood vessel growth, while focal laser therapy seals leaking vessels. For severe cases, vitrectomy surgery removes blood and scar tissue from inside your eye.
Remember that these treatments work most effectively when retinopathy is caught early.
Schedule a comprehensive eye exam at Chang Eye Group at one of our convenient locations in Pittsburgh to establish your personalized monitoring and treatment plan. Your eye doctor will determine the right screening schedule and intervention approach based on your current retinopathy stage and individual risk factors.
Protecting Your Vision from Diabetic Retinopathy Progression
Diabetic retinopathy may progress silently through its early stages, but you don’t have to wait for symptoms to appear before taking action. Throughout this guide, we’ve explored how this sight-threatening condition advances from invisible microaneurysms to vision-stealing complications, yet the power to protect your eyesight remains firmly in your control.
Blood glucose management serves as your strongest defense against retinopathy progression. When you maintain consistent control over your diabetes, you dramatically reduce your risk of advancing through the dangerous stages that lead to permanent vision loss. Blood pressure control and healthy lifestyle choices create additional layers of protection that work together to shield your retinal blood vessels from damage.
Early detection makes the difference between preserving your sight and losing it.
Regular dilated eye exams catch diabetic retinopathy before it reaches the advanced stages where complications like vitreous hemorrhage, retinal detachment, and neovascular glaucoma threaten your vision. People with type 1 diabetes should schedule their first screening within five years of diagnosis, while those with type 2 diabetes need immediate evaluation upon diagnosis.
Advanced treatments including anti-VEGF injections, laser therapy, and vitrectomy surgery can halt progression when prevention isn’t enough. These interventions work most effectively when diabetic retinopathy is detected early, before extensive damage occurs.
Your vision deserves protection at every stage of diabetes management. Don’t wait for floaters, blurred vision, or other warning signs to appear—by then, irreversible damage may have already occurred. The steps you take today determine whether you maintain clear sight or face preventable vision loss tomorrow.
Schedule your diabetic retinopathy screening at Chang Eye Group in Pittsburgh, where specialists can detect progression in its earliest stages and help preserve your sight for years to come.
FAQs
Q: What are the early signs of diabetic retinopathy?
A: Early signs of diabetic retinopathy often go unnoticed. The first detectable sign is usually the presence of microaneurysms, which appear as tiny red dots during an eye examination. Regular dilated eye exams are crucial for early detection, as symptoms may not be apparent in the initial stages.
Q: How does diabetic retinopathy progress to advanced stages?
A: Diabetic retinopathy progresses from mild to moderate to severe non-proliferative stages, and then to the proliferative stage. In advanced stages, new abnormal blood vessels grow, which can lead to complications such as vitreous hemorrhage and retinal detachment. The risk of severe vision loss increases significantly in these later stages.
Q: What are the symptoms of advanced diabetic retinopathy?
A: Advanced symptoms include more floaters, blurry or fluctuating vision, dark areas in your field of vision, poor night vision, faded colors, and potential vision loss. These symptoms typically appear after significant damage has already occurred to the retina.
Q: How can diabetic retinopathy be prevented or managed?
A: Prevention and management strategies include regular dilated eye exams, strict blood sugar control, managing blood pressure and cholesterol levels, maintaining a healthy weight, increasing physical activity, and quitting smoking. For advanced stages, treatments like anti-VEGF injections, laser therapy, and surgery may be necessary.
Q: How often should people with diabetes have eye exams?
A: The American Diabetes Association recommends that individuals with type 1 diabetes have their first dilated eye exam within 5 years of diagnosis, while those with type 2 diabetes should be examined at the time of diagnosis. Pregnant women with diabetes need more frequent monitoring starting in their first trimester. Regular screenings every six months are generally recommended for ongoing monitoring.